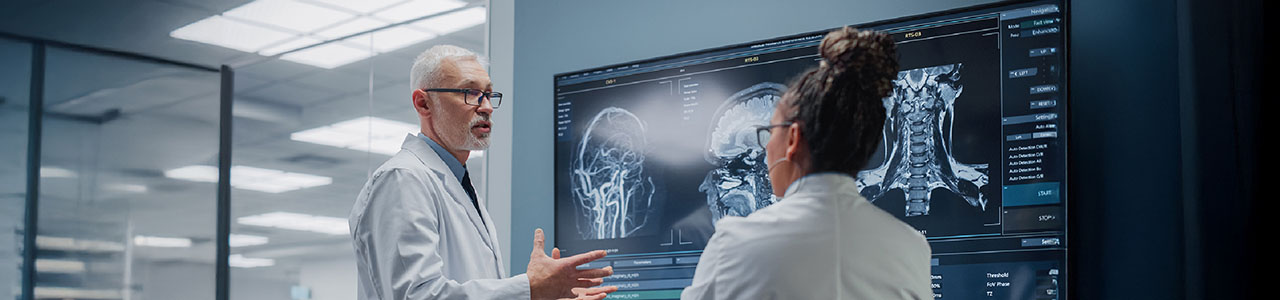
Multidisciplinary Head and Neck Cancers Symposium 2026 marks a pivotal moment in the battle against one of the most aggressive and devastating cancer types. The symposium is a comprehensive exploration of the latest advancements in head and neck cancer treatment, diagnosis, and survivorship.
The conference brings together leading experts from various disciplines, including radiation oncology, medical oncology, surgery, and more. Together, they will share insights and best practices to develop effective multidisciplinary approaches for treating head and neck cancers. From innovative diagnostic techniques to cutting-edge immunotherapies, the symposium promises to be a game-changer for patients and healthcare professionals alike.
Integrating Multidisciplinary Approaches in Head and Neck Cancer Treatment Strategies
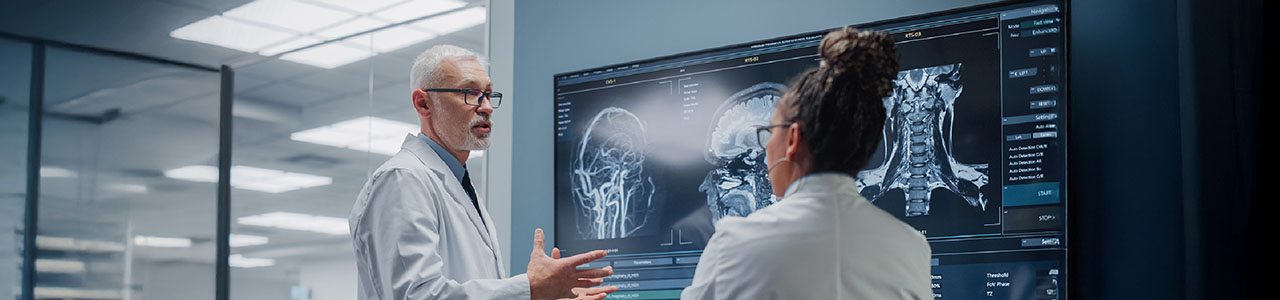
In recent years, head and neck cancer treatment has evolved significantly from traditional methods to a more patient-centered, multidisciplinary approach. This shift aims to improve treatment outcomes, reduce side effects, and enhance the overall quality of life for patients. By integrating different specialist disciplines, healthcare providers can offer more comprehensive and personalized care for individuals affected by head and neck cancers.
Examples of Successful Multidisciplinary Treatments
Successful multidisciplinary treatments for various stages of head and neck cancers typically involve a team of specialists working together to develop an individualized treatment plan. For example, in the case of oropharyngeal cancer, which affects the middle part of the throat, a multidisciplinary team may consist of an otolaryngologist (ENT surgeon), a medical oncologist, a radiation oncologist, a radiologist, and a dietitian. This team works together to provide personalized care, taking into account the patient’s medical history, disease stage, and lifestyle factors.
Examples of Multidisciplinary Treatments and Their Implications:
| Treatment Type | Specialist Discipline | Benefits | Challenges |
|---|---|---|---|
| Intensity-Modulated Radiation Therapy (IMRT) | Radiation Oncologist, Medical Oncologist | Improved precision and sparing of surrounding tissues, reducing side effects. | Potentially longer treatment times, higher costs. |
| Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy (HIPEC) | Surgical Oncologist, Medical Oncologist, Radiologist | Promising outcomes for advanced-stage peritoneal carcinomatosis, with improved survival rates and reduced recurrence. | Technical challenges, potential for organ damage or functional impairment. |
| Nanoparticle-Based Chemotherapy Delivery | Pharmacist, Medical Oncologist, Radiation Oncologist | Targeted delivery of chemotherapeutic agents, minimizing side effects and improving efficacy. | Expensive, need for advanced manufacturing and delivery capabilities. |
| Robotic-Assisted Surgical Oncology | Surgical Oncologist, Urologist, Otologist | Improved precision and dexterity, allowing for minimally invasive procedures and faster recovery. | Requires significant investment in technology and training, potential for technical issues. |
The Role of Immunotherapy in Combating Multidisciplinary Head and Neck Cancers: Multidisciplinary Head And Neck Cancers Symposium 2026
.png)
Immunotherapy, a revolutionary approach in cancer treatment, has shown remarkable potential in combating head and neck cancers. This multifaceted approach leverages the body’s immune system to identify and destroy cancer cells, offering new hope for patients battling this complex and aggressive disease. Recent studies have demonstrated the effectiveness of immunotherapy in improving overall survival rates and reducing recurrence in head and neck cancer patients.
Principles of Immunotherapy, Multidisciplinary head and neck cancers symposium 2026
Immunotherapy works by harnessing the body’s natural immune response to target cancer cells. It involves stimulating the immune system to recognize and attack cancer cells, thereby inhibiting tumor growth and preventing further metastasis. This approach differs significantly from traditional treatments, such as surgery and chemotherapy, which focus on killing cancer cells directly.
There are four primary types of immunotherapies:
1. Checkpoint inhibitors, including PD-1 and CTLA-4 inhibitors, which release the brakes on the immune system, allowing it to attack cancer cells more effectively.
2. Cancer vaccines, designed to stimulate the immune system to recognize and attack specific cancer cells.
3. Cytokines, which stimulate the immune system to produce chemical signals that activate immune cells to attack cancer cells.
4. CAR-T cell therapy, a type of adoptive immunotherapy where a patient’s T cells are genetically modified to recognize and attack cancer cells.
Types of Immunotherapies Currently Being Used or in Development for Head and Neck Cancer
Several immunotherapies have shown promise in treating head and neck cancer.
– Nivolumab (Opdivo), a PD-1 inhibitor, has demonstrated improved overall survival in head and neck cancer patients.
– Pembrolizumab (Keytruda), another PD-1 inhibitor, has shown increased overall survival and response rates in head and neck cancer patients.
– Cetuximab (Erbitux), a monoclonal antibody, has been used to treat head and neck cancer with EGFR expression.
– CAR-T cell therapy, currently in clinical trials, offers a promising new option for head and neck cancer treatment.
Mechanisms of Action for Various Immunotherapies
!A diagram illustrating the different mechanisms of action for various immunotherapies in treating head and neck cancers would be beneficial to visualize the process.
In this diagram, you would see four major sections highlighting the roles of each immunotherapy type:
– Checkpoint Inhibitors: releasing the brakes on the immune system to attack cancer cells
– Cancer Vaccines: stimulating the immune system to recognize and attack specific cancer cells
– Cytokines: stimulating the immune system to produce chemical signals that activate immune cells to attack cancer cells
– CAR-T cell therapy: genetically modifying a patient’s T cells to recognize and attack cancer cells.
Survivorship in Multidisciplinary Head and Neck Cancer Care

Surviving head and neck cancer is a significant achievement, but it brings a multitude of challenges that patients and healthcare providers must confront. The journey of survivorship is complex, involving not just the physical effects of treatment but also emotional and psychological impacts.
As we move forward in understanding the intricacies of head and neck cancer survivorship, it becomes imperative to acknowledge the multifaceted challenges that survivors encounter. This includes the need for comprehensive support systems that cater to their unique needs.
Physical Challenges
-
The recovery process post-head and neck cancer treatment is fraught with physical challenges. Some key areas include:
- The effects of radiation and surgery on the neck and throat can lead to chronic pain, difficulty in swallowing (dysphagia), and changes in vocal quality (dysphonia).
- The impact of chemotherapy and radiation on the mouth and throat can lead to xerosoma (dry mouth), oral infections, and dental decay.
- Loss of taste and smell can affect appetite and nutritional status, further impacting overall health and well-being.
- Nerve damage can lead to persistent numbness, tingling, and paralysis in affected areas.
To address these challenges, survivors require ongoing assessment, management, and supportive care. This includes regular check-ups with specialists such as ear, nose, and throat (ENT) surgeons, oncologists, and rehabilitation therapists.
Emotional Challenges
-
Survivors of head and neck cancer often experience heightened anxiety, depression, and post-traumatic stress disorder (PTSD) symptoms.
- The emotional distress of living through a cancer diagnosis, surgery, chemotherapy, and radiation therapy can be overwhelming.
- The fear of relapse and the knowledge that the disease has been invasive in their system can instill a deep-seated anxiety.
- The altered self-image and the stigma associated with physical changes can lead to feelings of insecurity and low self-esteem.
- The loss of independence due to decreased mobility, speech, and swallowing difficulties can further contribute to feelings of frustration and hopelessness.
Survivors need access to mental health professionals and emotional support services. Caregivers and loved ones also benefit from educational programs and support groups to better understand the survivor’s journey.
Support Systems
-
A comprehensive approach to survivorship involves addressing the emotional, social, and practical needs of survivors.
- Psychological counseling and therapy can provide a safe space to express feelings and address emotional trauma.
- Peer support groups allow survivors to share their experiences, build connections, and find mutual understanding.
- Community resources, such as meal delivery services, transportation assistance, and home care, can alleviate practical burdens.
- Online platforms and mobile apps can offer virtual support, education, and guidance to bridge the gap between clinical visits.
The most vital resource in this care network is the multidisciplinary team, made up of healthcare professionals from various disciplines who share knowledge and expertise to provide holistic support.
Ending Remarks
As we emerge from the Multidisciplinary Head and Neck Cancers Symposium 2026, we are equipped with a wealth of knowledge, insights, and strategies that will significantly improve patient outcomes and revolutionize head and neck cancer care. By embracing multidisciplinary approaches, we can offer patients hope, improved quality of life, and a promising future.
Frequently Asked Questions
What is the main goal of the Multidisciplinary Head and Neck Cancers Symposium 2026?
The main goal is to share the latest advancements in head and neck cancer treatment, diagnosis, and survivorship, with a focus on developing effective multidisciplinary approaches for treating head and neck cancers.
Who will participate in the symposium?
Leading experts from various disciplines, including radiation oncology, medical oncology, surgery, and more, will participate in the symposium.
What topics will be covered during the symposium?
The symposium will cover a wide range of topics, including innovative diagnostic techniques, cutting-edge immunotherapies, and comprehensive approaches to patient care.
What are the expected outcomes of the symposium?
The symposium promises to be a game-changer for patients and healthcare professionals, offering improved patient outcomes, better quality of life, and a promising future through the development of effective multidisciplinary approaches.
What is the significance of the symposium for head and neck cancer research?
The symposium represents a pivotal moment in the advancement of head and neck cancer research, bringing together leading experts to share insights, best practices, and strategies for improving patient outcomes.