As Medicare Advantage PPO plans 2026 takes center stage, this comprehensive guide aims to provide an in-depth understanding of the various aspects of these plans, shedding light on their benefits, limitations, and key features. With a focus on clarity and concision, this discussion will empower readers to make informed decisions about their healthcare options in 2026.
This in-depth exploration of Medicare Advantage PPO plans 2026 delves into the world of traditional Medicare and its differences from Medicare Advantage PPO plans, highlighting the advantages and disadvantages of each. By examining the features and benefits of these plans, including prescription drug coverage, dental, and vision care, readers will gain a deeper understanding of how Medicare Advantage PPO plans can help manage out-of-pocket costs and optimize their healthcare experience.
Evaluating Plan Providers and Network Coverage
Evaluating the right Medicare Advantage PPO plan provider and network coverage is a critical step in making informed decisions about your healthcare needs. With numerous plans and providers available, it can be overwhelming to determine which one best suits your requirements. Understanding the factors that contribute to a plan’s quality and coverage can help you make a more informed decision. In this section, we will explore the top Medicare Advantage PPO plan providers for 2026, how to assess the quality of a healthcare provider network, and the importance of evaluating a plan’s formulary.
Top Medicare Advantage PPO Plan Providers for 2026
When evaluating Medicare Advantage PPO plan providers, it is essential to consider customer satisfaction, network quality, and coverage. Based on these factors, the top Medicare Advantage PPO plan providers for 2026 are:
- UnitedHealthcare: With over 40 million members, UnitedHealthcare offers a wide range of Medicare Advantage PPO plans, including plans that provide enhanced benefits, such as dental, vision, and hearing coverage.
- Aetna: Aetna offers a variety of Medicare Advantage PPO plans that cater to different needs, including plans with lower premiums and higher deductibles.
- Cigna: Cigna offers Medicare Advantage PPO plans with a focus on preventive care, wellness programs, and online tools to help manage healthcare expenses.
- Anthem: Anthem offers Medicare Advantage PPO plans with a strong network of healthcare providers, including primary care physicians and specialists.
These providers have been recognized for their commitment to customer satisfaction, network quality, and coverage. However, it is essential to note that the best provider for you will depend on your individual needs and requirements.
Assessing the Quality of a Healthcare Provider Network
A healthcare provider network is a critical factor to consider when evaluating Medicare Advantage PPO plans. A network with a high-quality and diverse range of providers can ensure that you receive the best possible care. When assessing the quality of a healthcare provider network, consider the following factors:
- Access to specialists: Ensure that the network has a sufficient number of specialists in your area, including cardiologists, oncologists, and neurologists.
- Availability of out-of-network coverage: Consider plans that offer out-of-network coverage, either through a network of providers or a fee-for-service arrangement.
- Density of network providers: Look for plans with a high density of network providers in your area, ensuring that you have access to care when needed.
By carefully evaluating the quality of a healthcare provider network, you can ensure that you receive the best possible care.
The Importance of Evaluating a Plan’s Formulary
A plan’s formulary is a list of covered medications and the rules governing their use. When evaluating a Medicare Advantage PPO plan, it is essential to consider the formulary and any restrictions or limitations. A formulary should include the following:
- A comprehensive range of medications: Ensure that the formulary covers a wide range of medications, including common prescription drugs and specialty medications.
- Reasonable limitations and restrictions: Look for plans with reasonable limitations and restrictions, such as prior authorization requirements or step therapy protocols.
- No surprises clause: Look for plans that include a no surprises clause, which ensures that you are not surprised by unexpected costs or charges.
By carefully evaluating a plan’s formulary, you can ensure that you have access to the medications you need without unexpected costs or charges.
How to Research and Compare Plan Providers and Network Coverage
To research and compare plan providers and network coverage, use the following resources:
- Medicare Plan Finder: The Medicare Plan Finder is an online tool that allows you to compare Medicare Advantage PPO plans, their costs, and their benefits.
- Government websites: The Centers for Medicare and Medicaid Services (CMS) and the Medicare.gov website provide information on Medicare Advantage PPO plans, including their formularies and network providers.
- Insurance company websites: Visit the websites of insurance companies offering Medicare Advantage PPO plans to learn more about their plans, formularies, and network providers.
By using these resources, you can make an informed decision about which Medicare Advantage PPO plan is best for you.
Managing Prescription Medications and Costs

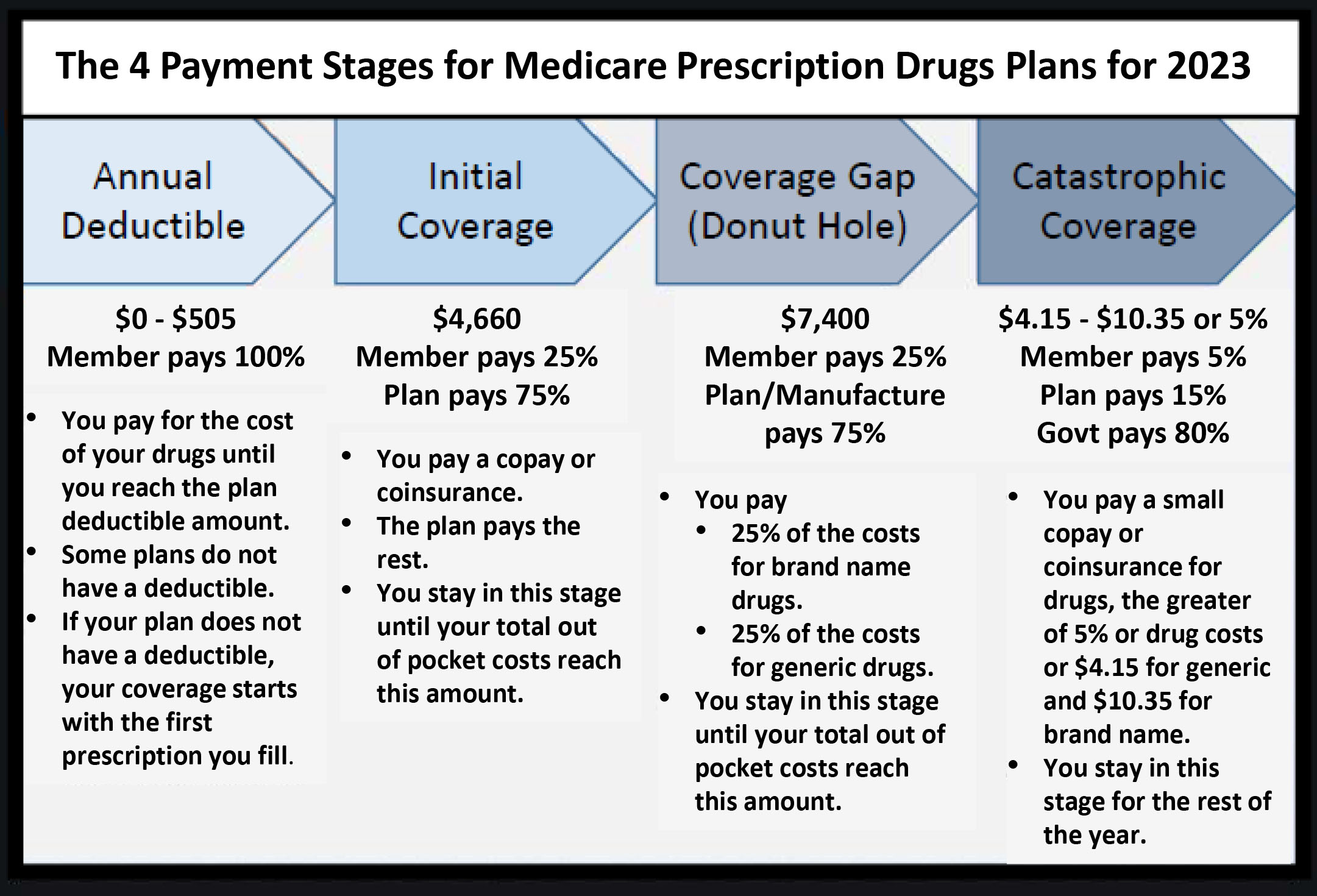
When it comes to managing prescription medications and costs, it’s essential to understand how Medicare Advantage PPO plans handle these expenses. These plans can vary in their coverage and cost-sharing structures, which can impact the amount you pay out-of-pocket for prescriptions.
Medicare Advantage PPO plans usually cover a range of prescription medications, including brand-name and generic drugs, except for specific exclusions stated in the plan’s list of covered medications. The cost-sharing for prescription medications typically consists of a copayment (copay) or coinsurance, plus any applicable deductible. The copay and coinsurance amounts can vary depending on the specific medication and the plan you’re enrolled in.
Copays, Coinsurance, and Deductibles
A copay is a fixed amount you pay for each prescription, usually $10 to $50. Coinsurance is a percentage of the prescription’s cost, typically ranging from 20% to 30%. The deductible, on the other hand, is the initial amount you pay each year before the plan begins to cover a portion of your prescription costs.
- Copays: $10 to $50 per prescription, depending on the medication and plan.
- Coinsurance: 20% to 30% of the prescription’s cost.
- Deductible: Initial cost-sharing requirement before the plan covers prescription medication expenses.
To minimize costs, many Medicare Advantage PPO plans offer medication management services, such as disease management programs and medication therapy management (MTM). These services aim to optimize medication use, improve adherence, and reduce unnecessary expenses.
Medication Management Services
Medication management services can significantly impact your prescription costs and overall healthcare expenses. These services typically involve a team of healthcare professionals working together to assess your medication regimen, identify potential issues, and develop strategies to optimize your medication use.
- Disease Management Programs (DMPs): Offer personalized guidance and support to help you manage chronic diseases, such as diabetes, heart failure, or asthma.
- Medication Therapy Management (MTM): A comprehensive service that involves:
- Medication review and optimization.
- Risk factor identification and monitoring.
- Patient education and counseling.
- Follow-up and ongoing support.
To further minimize prescription costs, it’s essential to explore various options, including coupons, patient assistance programs, and cost-sharing assistance.
Coupons, Patient Assistance Programs, and Cost-Sharing Assistance
Several programs can help you reduce your prescription expenses. Coupons, patient assistance programs, and cost-sharing assistance can be valuable resources to explore.
- Coupons: Manufacturer-provided discounts, often printable or digital, that can reduce copays or coinsurance.
- Patient Assistance Programs (PAPs): Services provided by pharmaceutical companies or organizations that offer free or low-cost medications for those who cannot afford them.
- Cost-Sharing Assistance: Some plans or programs may offer reduced or zero copays for certain medications or conditions, depending on your income or other factors.
When comparing Medicare Advantage PPO plans, it’s crucial to evaluate the coverage and costs of prescription medications, including any variations in coverage for special medications or treatments.
Coverage and Costs of Prescription Medications
The coverage and costs of prescription medications can vary significantly between Medicare Advantage PPO plans. Be sure to review each plan’s list of covered medications, copay and coinsurance amounts, and any applicable deductibles.
| Plan A | Plan B | Plan C | |
|---|---|---|---|
| Copay for Common Medications | $10 | $20 | $30 |
| Deductible for Prescription Medications | $100 | $200 | $300 |
| Coinsurance for Generic Medications | 10% | 20% | 30% |
Navigating Administrative Tasks and Enrollment
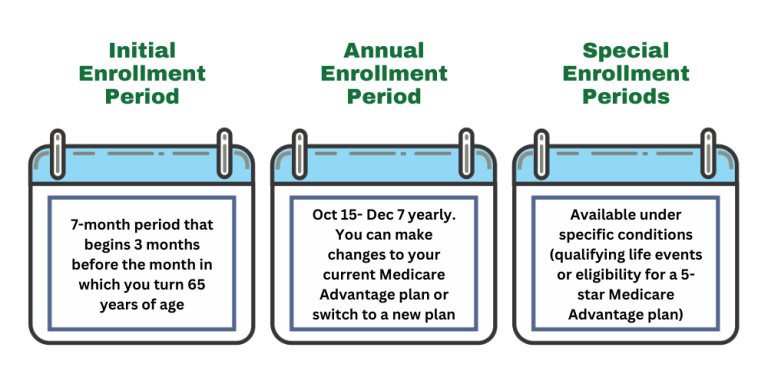
Enrolling in a Medicare Advantage PPO plan can be a bit overwhelming, but with the right guidance, you’ll be able to navigate the process with ease. It’s essential to understand the requirements and deadlines for initial enrollment or changing plans.
Medicare initial enrollment typically begins three months before your 65th birthday and ends three months after your birthday. However, if you’re eligible for Medicare due to disability, your initial enrollment period will be different. You can also change plans during the annual Open Enrollment Period, which usually takes place from October to December. Furthermore, some Medicare Advantage plans offer Special Enrollment Periods (SEPs) in specific circumstances, such as moving to a new location or losing other health coverage.
Enrollment Process, Medicare advantage ppo plans 2026
The Medicare enrollment process typically involves the following steps:
- Choosing a Medicare Advantage PPO plan that meets your healthcare needs and budget.
- Reviewing and comparing plans offered by different insurance providers.
- Understanding the plan’s benefits, including coverage for prescription medications, doctor visits, hospital stays, and other services.
- Enrolling in the chosen plan, either directly through the insurance company or through the Medicare website.
- Verifying your enrollment and plan details with the insurance provider.
- Setting up premium payments, if applicable.
It’s crucial to double-check the plan’s details and eligibility requirements before enrolling to avoid any confusion or delays.
Navigating the Medicare Plan Finder
The Medicare Plan Finder is an online tool that allows you to compare Medicare Advantage plans in your area. To use the tool effectively, follow these tips:
- Enter your zip code and Medicare information to access plan options.
- Filter plans by factors such as cost, coverage, and network providers.
- Review plan details, including benefits, deductibles, copays, and coinsurance.
- Compare plans from different insurance providers to find the best fit for your needs.
- Take advantage of the tool’s features, such as plan comparisons and cost estimates.
The Medicare Plan Finder is a valuable resource for finding the right Medicare Advantage PPO plan for your healthcare needs.
Administrative Tasks
Understanding plan-specific administrative tasks is crucial for a smooth Medicare experience. These tasks include:
- Filing claims for healthcare services and prescription medications.
- Accessing healthcare services, such as doctor visits, hospital stays, and emergency care.
- Communicating with plan providers, including phone, email, or online support.
- Managing premium payments, if applicable.
- Requesting and using medical records, including doctor notes and test results.
Being proactive and knowledgeable about these tasks can help you navigate any issues or challenges that may arise.
Common Administrative Issues
While rare, administrative issues can occur. Here are some examples and how to handle them:
- Lost documentation: If you’ve misplaced a document, such as a claim receipt or insurance card, contact your plan provider to request a replacement.
- Denied claims: If a claim is denied, review the decision with your plan provider to understand the reason and resolve the issue.
- Billing errors: If you’ve received an incorrect bill, contact your plan provider to dispute the error and correct the billing information.
Proactively addressing these issues can help you avoid delays or complications in your healthcare treatment.
Understanding Out-of-Network Coverage and Exceptions
Understanding your Medicare Advantage PPO plan’s out-of-network coverage is crucial to making informed decisions about your healthcare. While many medical services are covered within the plan’s network, there may be situations where you need to seek care outside of it. In this section, we’ll explore the rules and exceptions for out-of-network coverage under Medicare Advantage PPO plans, including emergency or urgent care services.
Medicare Advantage PPO plans often offer out-of-network coverage for medically necessary services, but the extent of coverage and costs can vary depending on the plan. Typically, these plans require you to pay a higher copayment or coinsurance for out-of-network services compared to in-network services. However, in emergency or urgent situations, such as a heart attack or severe injury, you’re usually able to receive necessary treatment without prior notification or approval.
Emergency and Urgent Care Services
Emergency or urgent care services are typically covered under Medicare Advantage PPO plans without requiring prior approval or notification. This includes services for conditions that require immediate attention, such as stroke, heart attack, or severe injuries. You’re usually able to receive treatment at any healthcare facility without worrying about out-of-network costs.
Examples of Out-of-Network Coverage
There are several situations where out-of-network coverage might be necessary:
–
Emergency Care Outside Your Network
+ When you’re traveling and don’t have access to your plan’s network.
+ When you’re in an area with limited network providers.
+ In cases of unexpected medical emergencies.
–
Short-Term Care Outside Your Network
+ When you’re receiving short-term care for a condition that’s not immediately life-threatening.
+ When your plan network provider is unavailable or on vacation.
Navigating Out-of-Network Coverage
To navigate out-of-network coverage, follow these steps:
1. Verify your insurance coverage: Before seeking care, verify your insurance coverage with your Medicare Advantage PPO plan to understand any out-of-network costs or limitations.
2. Prior Authorizations: For services not immediately life-threatening, you might need prior authorization from your plan before receiving out-of-network care. This ensures that your plan covers the service and helps you avoid additional costs.
3. Referrals to Specialty Care: If you need specialty care, such as a specialist or hospitalization, your primary care physician may need to refer you to an in-network specialist or facility. If this isn’t possible, you can seek care from an out-of-network provider, but be aware of potential costs and limitations.
4. Keep records: Keep accurate records of all out-of-network care, including dates, services, and costs. This will help you track your expenses and ensure you receive the coverage you’re entitled to.
Out-of-Network Costs and Limits
When seeking care outside your Medicare Advantage PPO network, you may be responsible for paying higher copayments or coinsurances than you would for in-network services. These costs can add up quickly, so it’s essential to understand your plan’s coverage limits and any out-of-pocket maximums.
In conclusion, while Medicare Advantage PPO plans offer out-of-network coverage for emergency or urgent care services, it’s crucial to understand your plan’s coverage rules and exceptions. By being informed and prepared, you can make the most out of your healthcare benefits.
Conclusion: Medicare Advantage Ppo Plans 2026
In conclusion, Medicare Advantage PPO plans 2026 offer a range of benefits and features that cater to the diverse needs of seniors and individuals with disabilities. By navigating the complexities of these plans, readers will be better equipped to make informed decisions about their healthcare options and maximize their coverage and benefits. Whether you’re seeking prescription drug coverage, dental, or vision care, Medicare Advantage PPO plans 2026 provide a comprehensive solution for managing out-of-pocket costs and optimizing your healthcare experience.
FAQ Guide
What is a Medicare Advantage PPO plan?
A Medicare Advantage PPO plan is a type of Medicare Advantage plan that offers a network of healthcare providers and hospitals, but also allows for out-of-network coverage at a higher cost-sharing level.
What are the benefits of Medicare Advantage PPO plans?
Medicare Advantage PPO plans offer benefits such as prescription drug coverage, dental, and vision care, as well as out-of-network coverage options.
Certain requirements must be met to be eligible for Medicare Advantage PPO plans, including being age 65 or older or being disabled and receiving Medicare.